Can Osteoporosis Be Reversed?
“Can Osteoporosis Be Reversed?“ was written by Oregon Health Sciences dietetic intern Rachel Moore. Edited/reviewed by Katie Dodd, MS, RDN, CSG, LD, FAND.
What is Osteoporosis?
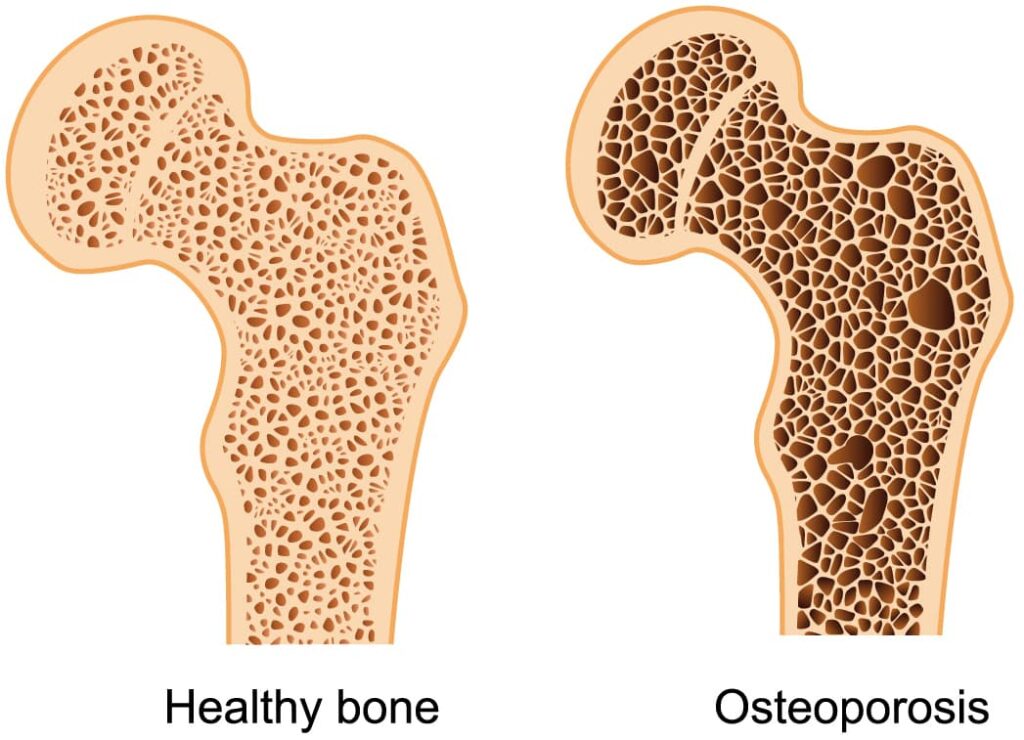
Osteoporosis is a bone disease that shows decreased bone mineral density and bone mass. In other words, osteoporosis is a disease that weakens bones and makes them more porous (making them more fragile than healthy bones).
Osteoporosis can increase your risk of bones breaking, especially in the wrist, spine, and hip. It is estimated that 1 in 3 women and 1 in 5 men suffer from a broken bone as a result of osteoporosis.
Now, let’s get right to the question at hand: can osteoporosis be reversed? The short answer is no. But the right treatment, nutrition, exercise, and lifestyle change can help strengthen your bones and protect them from breaks!
Osteoporosis Symptoms
Many people get osteoporosis without even knowing it. You may not see any symptoms until you break a bone. Sometimes, people aren’t diagnosed with osteoporosis even after they break a bone.
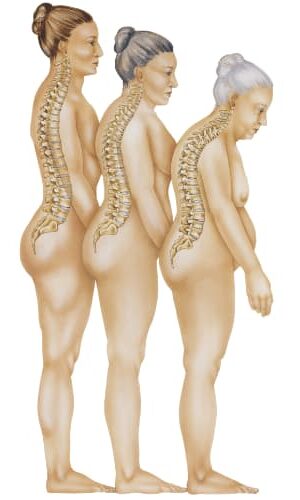
If you get a broken bone after a small fall (like falling from standing or from bumping into something), then this may be a sign that you have osteoporosis. Osteoporosis in the vertebra (also known as back bones) can lead to vertebrae collapse, and can then lead to:
- Sloping shoulders
- Curved back
- Loss of height
- Back pain
- Hunched posture
With osteoporosis, normal activities such as bending, lifting, and climbing stairs can lead to bone breaks. Talk to your doctor if you have any of these symptoms.
Diagnosing Osteoporosis
An early diagnosis of osteoporosis can help protect against more broken bones.
The best way to diagnose osteoporosis is with a bone mineral density test. A bone mineral density test measures the amount of bone mineral in your bones and compares it to the average healthy young adult.
The results of this test tell you how strong your bones are, if you have osteoporosis, and what your risk is for getting a broken bone.
Women are at a higher risk for osteoporosis. Therefore, it’s recommended that women get screened when they are over the age of 65 or if they are under the age of 65 with increased risk.
What Causes Osteoporosis?
Many different factors can lead to osteoporosis.
Osteoporosis Risk Factors
- Age: Older adults are more likely to get osteoporosis. As we age, our bones naturally become thinner.
- Sex: Women lose bone more quickly after menopause because the production of estrogen slows down.
- Family History: Your chances of developing osteoporosis increase if you have a family history of osteoporosis or hip fractures.
- Body Size: Slender, thin women and men have a greater risk for developing osteoporosis because they have less bone compared to larger individuals.
- Race: White and Asian American women are at a higher risk compared to Mexican American and Black American women. White men are at a higher risk compared to Black American and Mexican American men.

Medications That Cause Osteoporosis
Some medications can impact bone strength and density when used long-term. If you are taking one of the following medications, talk to your doctor about how to prevent excessive bone loss.
- Glucocorticoids: These steroids are usually taken to treat autoimmune disorders (such as rheumatoid arthritis, ulcerative colitis, and eczema), allergies, asthma, adrenal insufficiency, and heart failure.
- Thyroid Replacement Therapy medications
- Certain drugs used to treat diabetes
- Proton pump inhibitors
- Certain antidepressants and sedatives
- Certain immunosuppressants
- Aromatase inhibitors (used to treat breast cancer)
- Certain antipsychotics
- Certain anticonvulsants and anti-epileptics
- Anti-coagulants
Diseases and Conditions That Cause Osteoporosis
Some diseases and conditions may increase your risk for osteoporosis. If you have a history of one of the following, talk to your doctor about ways to protect bone strength.
- Autoimmune Disorders: rheumatoid arthritis, lupus, ankylosing spondylitis
- Gastrointestinal Diseases: lactose intolerance, Crohn’s inflammatory bowel disease, celiac disease
- Cancer: breast cancer, prostate cancer
- Surgery: gastrectomy, gastrointestinal bypass procedure, organ transplants
- Neurological Disorders: stroke, Parkinson’s disease, multiple sclerosis, spinal cord injuries
- Blood Disorders: leukemia and lymphoma, multiple myeloma, sickle cell disease, thalassemia
- Endocrine/Hormonal Disorders: diabetes, hyperparathyroidism, hyperthyroidism, Cushing’s syndrome, thyrotoxicosis, irregular periods, premature menopause, low levels of testosterone and estrogen in men
- Mental Illness: depression, eating disorders
- Other Diseases: AIDS/HIV, chronic obstructive pulmonary disease (COPD), emphysema, female athlete triad (includes loss of menstrual periods, an eating disorder and excessive exercise), chronic kidney disease, liver disease, polio and post-polio syndrome, poor diet (including malnutrition), scoliosis, weight loss
Lifestyle Factors That May Lead to Osteoporosis
Nursing Home
Living in a nursing home or long-term care facility can put older adults at high risk for osteoporosis and broken bones.
This is because of high risk factors such as: older age, decreased physical function, poor muscle strength, poor nutrition, decreased cognition, dementia, and taking multiple medications.
Alcohol and Smoking
Excessive alcohol consumption is another risk factor for osteoporosis and can also lead to more falls. Additionally, research shows that those who smoke lose bone density faster than those who don’t smoke.
Lifestyle
Finally, poor diet and inactivity can also lead to osteoporosis. If we don’t give bones the nutrients that they need and don’t use them as much as we can, then we’re more likely to have weak bones and broken bones.

Can Osteoporosis Be Reversed?
The short answer is no, osteoporosis can’t be reversed. Once your bones become porous from osteoporosis, you can’t fix them make them more “dense.” But, you can strengthen your bones to prevent fractures and further bone loss.
Treatment, nutrition, exercise, and lifestyle change can help strengthen your bones and prevent broken bones.
How Can You Prevent and Treat Osteoporosis?
Even though you can’t reverse osteoporosis, there are steps you can take to prevent more damage to your bones. Always work with your healthcare team to figure out a plan that’s right for you.
Nutrition for Osteoporosis
Good nutrition is very important to maintain bone health and prevent early bone loss. Nutrients such as calcium, vitamin D, and protein are especially important for bone strength!
Calcium
Calcium is necessary for preventing and treating osteoporosis. Our bones contain 99% of our body’s calcium. Our bones store the calcium to help keep enough of it in our blood. We need calcium for bone strength and nerve and muscle function.
When we don’t get enough calcium from our diet, our bones push calcium back into the blood to maintain muscle and nerve function. If we regularly don’t get enough calcium, then our bones become weak as they continue to push the calcium from our bones back into the blood.
Over time, this can lead to osteoporosis.
To help prevent osteoporosis, it is recommended that women over the age of 50 consume 1200 mg of calcium a day, and men over the age of 50 consume 1000 mg of calcium a day. Anyone over the age of 70 should consume 1200 mg of calcium a day.
Foods that are high in calcium include milk and dairy products, green vegetables, fruits, and nuts.
Calcium can also be fortified in foods such as bread, cereals, fruit juices, and non-dairy milk. (Fortified means that a nutrient is added to a food that doesn’t normally have that nutrient in it).
Eating a well-balanced diet can help you consume enough calcium. However, if you are unable to consume the recommended amount through food alone, then you can supplement with 500-600 mg of calcium a day.
Calcium supplementation should be combined with vitamin D-rich foods or a vitamin D supplement for adequate absorption. Talk to your doctor or a registered dietitian to discuss what’s right for you.

For more foods high in calcium, check out our High Calcium Food Chart article.
Vitamin D
Vitamin D is needed for calcium to absorb. Therefore, high enough vitamin D levels are important for protecting bone strength. Vitamin D also helps with bone renewal, bone mineralization, and it helps keep our muscles strong.
Did you know that we get 70-80% of our needed vitamin D from the sun? Vitamin D is made when our skin is exposed to UV- B sunlight.
Since only a few foods contain vitamin D, our best way for supporting necessary vitamin D levels is through sunshine. Aim for 10-20 minutes of sunshine between 10 a.m. and 2 p.m.
Foods high in vitamin D include salmon, sardines, tuna, shitake mushrooms, and egg yolk.
If you can’t get enough sun, then you can supplement with vitamin D. It is recommended that anyone over the age of 60 consume 800-1000 IU a day to keep or improve their bone strength.
Protein
Protein is another important nutrient for protecting our bone and muscle strength. Muscle strength is important for preventing falls, which often leads to broken bones.
Foods high in protein include lean red meats, poultry, turkey, dairy, eggs, beans, and nuts.
Exercise for Osteoporosis
Bones and muscles get “stressed” during weight-bearing exercise. Examples of weight-bearing exercise include walking, dancing, elliptical machines, and low-impact aerobics. This is actually a good thing because they respond to the “stress” by getting stronger.
Exercise can also help with balance, which then helps prevent falling. It is reported that one-third of people over 65 experience a fall each year. Studies have shown that exercise can reduce the risk of falls by almost 25%!
It has also been suggested that exercise improves function and delays loss of independence.
Medications to Treat Osteoporosis
If you have osteoporosis, your doctor may suggest medication(s) in addition to nutrition, exercise, and lifestyle changes.
Medications often used to treat osteoporosis include:
- Bisphosphonates (alendronate, risedronate, ibandronate, zoledronic acid)
- Raloxifene and bazedoxifene
- Teriparatide and abaloparatide
- Denosumab
- Romosozumab
- Hormone Replacement Therapy (used for menopausal women)
Conclusion: Can Osteoporosis Be Reversed?
While osteoporosis can’t be reversed, proper nutrition, exercise, and lifestyle changes can help strengthen your bones. Talk to your doctor or a registered dietitian about ways you can improve your diet and lifestyle to lower your risk for fractures.

References
- What is Osteoporosis? International Osteoporosis Foundation. https://www.osteoporosis.foundation/patients .
- What is Osteoporosis and What Causes It? Bone Health & Osteoporosis Foundation. https://www.nof.org/patients/what-is-osteoporosis/.
- Osteoporosis Overview. The NIH Osteoporosis and Related Bone Diseases National Resource Center. https://www.bones.nih.gov/health-info/bone/osteoporosis/overview.
- Osteoporosis. US Department of Health & Human Services: Office on Women’s Health. https://www.womenshealth.gov/a-z-topics/osteoporosis.
- Osteoporosis prevention, diagnosis and therapy. Journal of the American Medical Association. 2001;285(6),785-95. https://pubmed.ncbi.nlm.nih.gov/11176917/.
