“Osteoporosis in the Elderly” was written by Arantza Barroso. Edited/reviewed by Katie Dodd, MS, RDN, CSG, LD, FAND. Arantza is a dietetic intern at Oregon Health Sciences University.
Osteoporosis can occur at any age. However, the risk of developing this “silent disease” increases as we get older.
Osteoporosis in the elderly is a major cause of broken bones. Fractures can lead to hospitalization, poor healing, and loss of independence. But there are steps that can be taken to help prevent fractures and maintain a good quality of life.

What is osteoporosis?
By definition, osteoporosis means “porous bone”.
Although all bones are porous, osteoporosis causes the little pores in the bones to be much larger than they should be. Therefore, they become less dense and more fragile than normal bones.
Osteoporosis is a common chronic disease that develops as humans age. It is often considered a “silent disease” because most people do not feel any symptoms of bone weakening. That is until there is an unexpected break or fracture involved.
Fractures are serious complications of osteoporosis in the elderly. Therefore, it is crucial to avoid them in order to preserve the quality of life of older adults.
What causes osteoporosis?
In the life cycle of bones, two things are generally occurring:
- Bone tissue is broken down by certain cells to release minerals such as calcium.
- Other cells are in charge of rebuilding the tissue that is lost.
As we age, that ratio of breaking down and rebuilding begins to change. As such, more bone tissue is lost and less is being rebuilt.
Without the minerals needed to rebuild the bone tissue, the bones become soft. Unfortunately, this makes them more fragile and easier to break.
There are many things that can increase the likelihood of developing osteoporosis including:
- autoimmune disorders
- gastrointestinal disorders
- hormonal disorders
- some medications
- even pregnancy
It is important for older adults and/or their caregivers to talk to their doctors. And ask if there are any underlying conditions that may contribute to bone loss. (1)
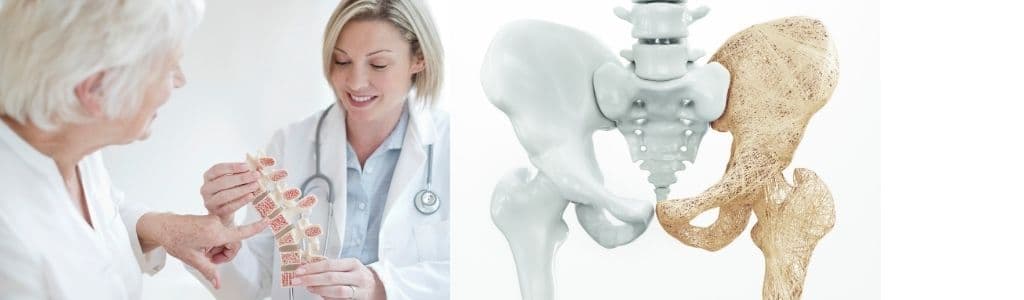
Osteoporosis in the Elderly
Bones that are weakened by osteoporosis are more likely to fracture than normal bones. As such, sudden unexpected fractures are usually due to the development of osteoporosis in the elderly.
These fractures may pose significant problems for the elderly. Unfortunately, bones that have already been weakened are less likely to reach full recovery. This slow recovery can lead to a decrease in overall quality of life. It can lead to long-term disability and loss of independence.
Who is at risk?
There are many risk factors for osteoporosis in the elderly. Some are controllable, while others are not.
Risk Factors for Osteoporosis
Risk factors for osteoporosis that you cannot control include:
- Age
- After the age of 30, bone tissue breaks down at a higher rate than it is being rebuilt. This causes loss in bone density.
- Sex
- Women are more likely to develop osteoporosis.
- Men are at high risk for osteoporosis after the age of 70.
- Genetics
- Family history of low bone density or osteoporosis may increase risk of osteoporosis.
- Other diagnoses:
- In some cases osteoporosis caused by an underlying health condition- is increased if the underlying condition is not treated or managed.
- Menopause
- Women are more likely to develop osteoporosis due to hormonal changes during menopause. A hormone called estrogen is part of the process of rebuilding bones. And estrogen levels in women are significantly lower after menopause.
- Low levels of testosterone in males
- Although men do not go through rapid hormonal changes, low testosterone levels can lead to the development of osteoporosis. Click here for more information on testosterone deficiency and osteoporosis.
- Race
- Osteoporosis affects women and men of all races. However, it is most common in non-hispanic white women and men.

Controllable Risk Factors for Osteoporosis
Other factors that increase the risk for the development of osteoporosis are controllable. Such factors include:
- Diet
- A long-term diet low on protein, calcium, and vitamin D (nutrients important for bone health!).
- Sedentary lifestyle
- Exercise is important for the strengthening of muscles and bones.
- Alcohol
- Long-term excessive drinking can interfere with the rebuilding of bones. Therefore, causing loss of bone density.
- Nicotine
- Tobacco use can inhibit bone growth, increasing the risk for osteoporosis (2).
Impacts on the elderly – Signs and symptoms to look for
Unfortunately, in most cases, there are no physical signs of osteoporosis in the elderly. However, sudden fractures can happen unexpectedly. It is important to recognize the symptoms of fractures quickly.
Symptoms of fractures on spinal vertebrae (the back!) include:
- severe back pain
- loss of height
- changes in posture related to pain.
Osteoporosis-related fractures are most common on the hips, the wrists, and spinal vertebrae.
These are usually caused by minor falls or even normal movements such as bending over or lifting something from the floor (3).
These fractures can lead to a significant decline in the quality of life of older adults. Unfortunately, these fractures are difficult to recover from. They can cause more health issues. And they can be costly!

Osteoporosis Statistics
Osteoporosis is a major public health issue in the United States. About 10.2 million American men and women over 50 years of age were diagnosed with osteoporosis as of 2010. And, over 80% of those cases were women (4).
Women are more likely than men to experience fractures at a younger age. In turn, this greatly increases the rates of disability among older women.
A research study looked at the likelihood of women having repeat fractures. They found that 10% had another fracture within a year. Another 18% had another fracture within 2 years. And finally, 31% had another fracture within 5 years (5).
Screening and Diagnosis
Research suggests that screening for osteoporosis should begin at the age of 65 for women. However, if a woman under 65 is at an increased risk of osteoporosis, she should be screened as recommended by her doctor.
So far, there are no established recommendations regarding when men should be screened for osteoporosis. But, it is generally suggested to report any fractures, family history, medical conditions, etc. to their doctors during annual checkups. Doctors will also perform a physical exam to aid in the diagnosis of osteoporosis.
The bone mineral density (BMD) test is used to measure bone density in specific areas (usually the hips and the spine). This can helps to accurately diagnose osteoporosis. And to monitor how well treatments are working.
The most common test that is used to diagnose osteoporosis is the dual energy x-ray absorptiometry (DEXA). A T-score equal to or lower than a -2.5 indicates osteoporosis-level bone density.
How can I manage my osteoporosis?
Since the bones are constantly breaking down and rebuilding, it is possible to manage osteoporosis and increase bone density.

Calcium and Osteoporosis
Calcium is a mineral that is essential for the human body to function. If we don’t get this nutrient through food, our bodies will still find a way to get it.
Most calcium (about 99%) is stored in bones and teeth. If there is not enough calcium coming from the diet, the body will take calcium from the bones. Calcium is needed for lots of functions in the body, including blood clotting and muscle contraction (6).
It is crucial to consume enough calcium through diet to protect the bones. Calcium supplements may be needed for those who cannot get enough calcium from food alone. Talk to your doctor before starting any supplements.
How Much Calcium?
Men and women need different amounts of calcium.
Women:
- Age < 50 = 1,000 mg/day
- Age 51+ = 1,200 mg/day
Men:
- Age < 70 = 1,000 mg/day
- Age 71+ = 1,200 mg/day
Food Sources of Calcium
Recommended foods high in calcium include:
- dairy products: yogurt, milk, and cheese
- Fortified foods and beverages: orange juice (fortified with calcium and vitamin D), and cereals
- Almonds
- Turnip greens
- Bok Choi
- Kale
Notice that many food sources of calcium that are commonly recommended such as spinach, collard greens, and sweet potatoes are not present in the list above. That is because these foods contain a compound called oxalic acid that decreases the absorption of calcium.
Fortified foods and beverages (with calcium added) are other options.
Click here for more information on calcium and calcium-rich foods.

Vitamin D and Osteoporosis
Vitamin D helps the body absorb calcium. A vitamin D deficiency can increase the risk of bone fractures and the development of osteoporosis.
There are three ways to obtain vitamin D:
- sunlight
- food
- supplements.
The skin is able to make vitamin D from sunlight. The amount of vitamin D that can be made by the skin varies by age, skin pigmentation, latitude, time of day, etc. (6)
Other factors include:
- Increasing Age
- Aging skin gradually loses the ability to make vitamin D.
- Wearing SPF
- SPF as low as 8 can reduce vitamin D production by 95%
- Risk of skin cancer
- Extensive exposure to sunlight can significantly increase risk of developing skin cancer
- Living in cities/institutional settings like nursing homes
- More time is spent indoors
How Much Vitamin D
The recommended amount of vitamin D is:
- <50 years old: 600 IU daily
- 71+ years old: 800 IU daily
Research has shown that vitamin D supplementation can help decrease bone turnover and increase bone density. However, too much vitamin D can have adverse effects (7).
Talk to a doctor or healthcare provider to assess your vitamin D level. And to suggest appropriate ways to fix a deficiency.
Food Sources of Vitamin D
Unfortunately, the availability of vitamin D in food is very limited. Fatty fish like salmon, tuna, and mackerel are good sources of vitamin D, as well as eggs and fortified foods such as milk, orange juice, soymilk, and cereals.
Check out this article for more information on Vitamin D in the Elderly.
Exercise and Osteoporosis
Resistance training and exercises like walking and jogging are helpful in building and strengthening muscle mass. Additionally, they can improve balance and coordination. Weight-bearing exercises are recommended for bone health and to help avoid fractures from falls.
By improving strength and coordination, older adults are able to move and fulfill daily activities with less risk of falling, as well as delay loss of independence(8).
Physical therapists and rehabilitation specialists can help older adults develop a specific routine of exercises. Additionally, it is important to discuss exercise with your healthcare team.
Working with a Dietitian
Dietitians are able to provide nutrition education that is crucial in the management of osteoporosis. A dietitian can help in making healthy food choices. Similarly, they can help with choosing supplements to fill nutrition gaps.
Proper nutrition is crucial in the management of osteoporosis to prevent further bone loss and maintain the quality of life of older adults.

Working with Your Healthcare Team
If you have osteoporosis it is so important to work with your healthcare team.
Many healthcare providers work together to provide comprehensive treatments for osteoporosis (3). These specialties include:
- Endocrinologists
- Gynecologists
- Geriatricians
- Occupational therapists
- Physical therapists
- Primary care provider
- Registered dietitian
The team of healthcare providers work together to manage all aspects of osteoporosis treatment. For example, nutrition, medicine, physiological treatments, and more. The goal is to help those with osteoporosis to maintain the best quality of life possible.
Communication between the patient and the healthcare team is important to determine the best treatment option for each individual patient.
Preventing falls and fractures in the elderly
Falls and fractures can lead to further medical complications and cause older adults to lose their independence.
Staying physically active, limiting alcohol and tobacco consumption, and maintaining a diet rich in calcium and vitamin D are very important to improve or maintain bone and muscle strength and avoid falls. (8)
Other ways to avoid falls and fractures include efforts to control the environment. Physical therapists and occupational therapists can assist with preventing falls in the home.
Maintaining safe conditions
It is important to consider maintaining safe conditions inside and outside the home to prevent falls.
Tips to prevent falls at home:
- Keeping rooms free of clutter and avoiding having multiple things on the floors.
- Wearing supportive, non-slip shoes indoors.
- Using a rubber mat in the shower or tub to prevent slipping.
- Adding more lights in the home such as nightlights in the bedrooms, and ceiling fixtures to keep stairs well-lit.
- Being mindful of where carpets and rugs are placed.
- Installing handrails by stairs.
Tips to prevent falls outside of the home:
- Wearing supportive, non-slip shoes.
- Avoid walking on wet or slippery sidewalks.
- Using a cane for stability.
- Being mindful of curbs and steps when walking outdoors. (9)
Improved Quality of Life
Management of osteoporosis helps older adults to keep their independence and increase their confidence.
The goal of osteoporosis management is to maintain or even improve the quality of life of older adults. Simialarly, to delay disability and help them live the life that they desire.
Seeking treatment as early as possible and adhering to the advice of healthcare professionals is so important.
Maintain regular checkups with your healthcare team. Ask them about potential risk factors that may affect bone health. Or increase the chances of falling.
Osteoporosis in the Elderly – Conclusion
Osteoporosis in the elderly is fairly common. And it can have a negative impact on quality of life.
But, the good news is there are steps that can be taken to maintain bone health. And to prevent falls and fractures.
Here are some additional resources to help:
Resources
More helpful resources for older adults with osteoporosis:
- National Osteoporosis Foundation
- American Bone Health
- International Society for Clinical Densitometry
- National Institutes of Health Osteoporosis and Related Bone Diseases National Resource Center
References
- National Osteoporosis Foundation. (2021, April 12). Learn what osteoporosis is and what it’s caused by. National Osteoporosis Foundation. https://www.nof.org/patients/what-is-osteoporosis/.
- Curtis, S. (n.d.). Who is at risk for osteoporosis? Spine-Health. https://www.spine-health.com/conditions/osteoporosis/who-risk-osteoporosis.
- U.S. Department of Health and Human Services. (2019, October). Osteoporosis overview. National Institute of Arthritis and Musculoskeletal and Skin Diseases. https://www.bones.nih.gov/health-info/bone/osteoporosis/overview.
- Key statistic for North America: International Osteoporosis Foundation. IOF International Osteoporosis Foundation. (n.d.). https://www.osteoporosis.foundation/facts-statistics/key-statistic-for-north-america.
- Balasubramanian, A., Zhang, J., Chen, L., Wenkert, D., Daigle, S. G., Grauer, A., & Curtis, J. R. (2018). Risk of subsequent fracture after prior fracture among older women. Osteoporosis International, 30(1), 79–92. https://doi.org/10.1007/s00198-018-4732-1
- National Osteoporosis Foundation. (2018, February 26). Calcium/Vitamin D REQUIREMENTS, Recommended foods & Supplements. National Osteoporosis Foundation. https://www.nof.org/patients/treatment/calciumvitamin-d/.
- Lips, P., & van Schoor, N. M. (2011). The effect of vitamin d on bone and osteoporosis. Best Practice & Research Clinical Endocrinology & Metabolism, 25(4), 585–591. https://doi.org/10.1016/j.beem.2011.05.002
- U.S. Department of Health and Human Services. (2017, June 26). Osteoporosis. National Institute on Aging. https://www.nia.nih.gov/health/osteoporosis.
- Cleveland Clinic. (2020, April 27). Osteoporosis: Symptoms, causes, tests & treatment. Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/4443-osteoporosis.
